 |
 |
 |
 |
|
 |
 |
 |
 |
 |
 |
 |
 |
||
 |
||||
Cross-Arch Extrusion
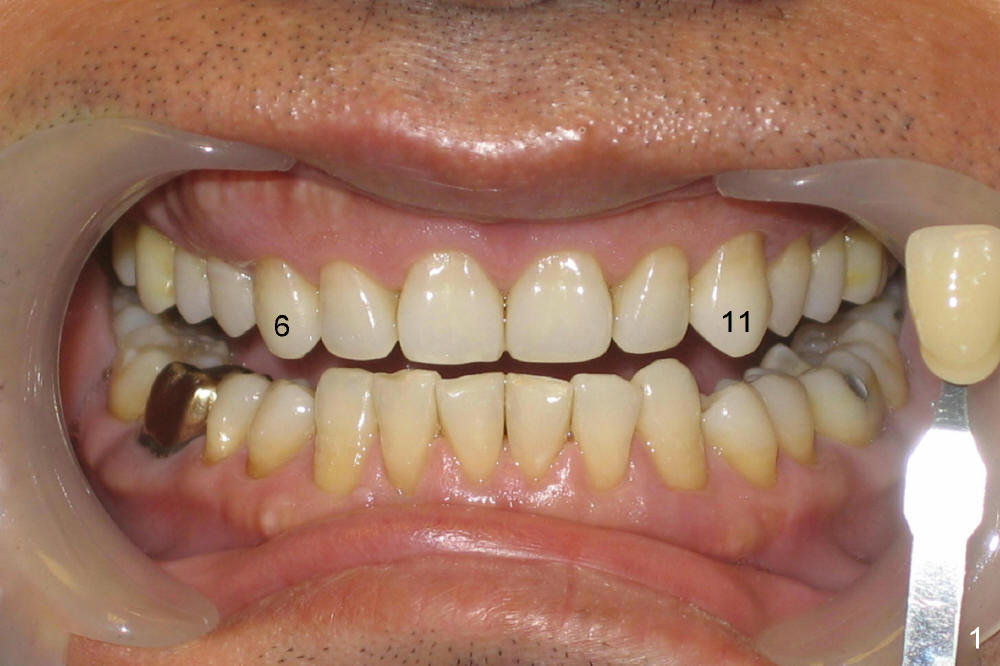
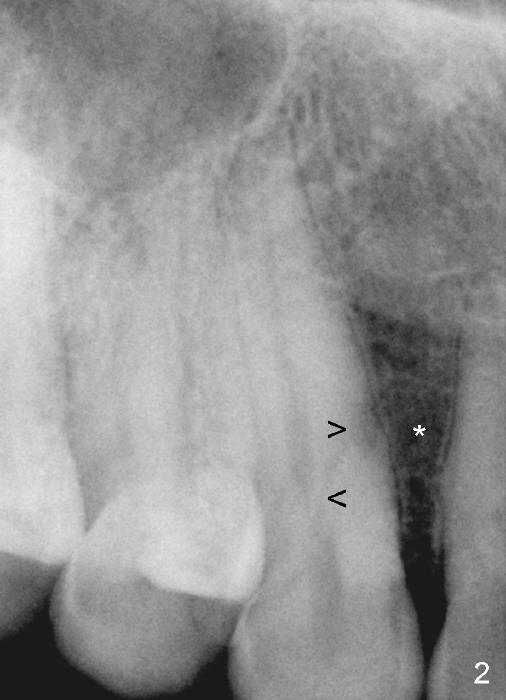
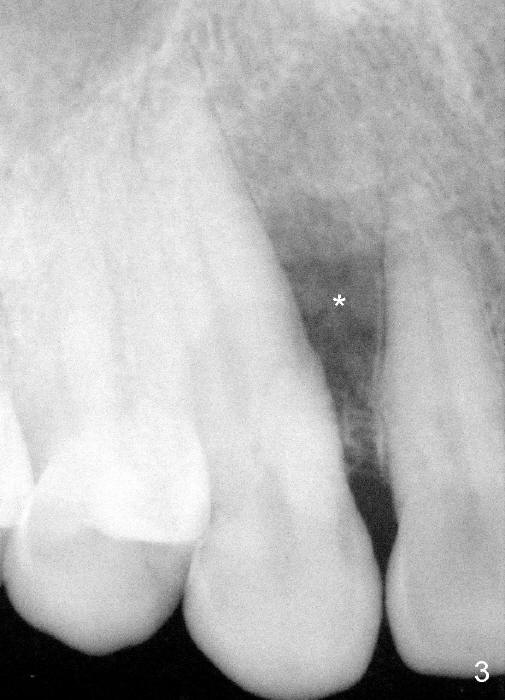
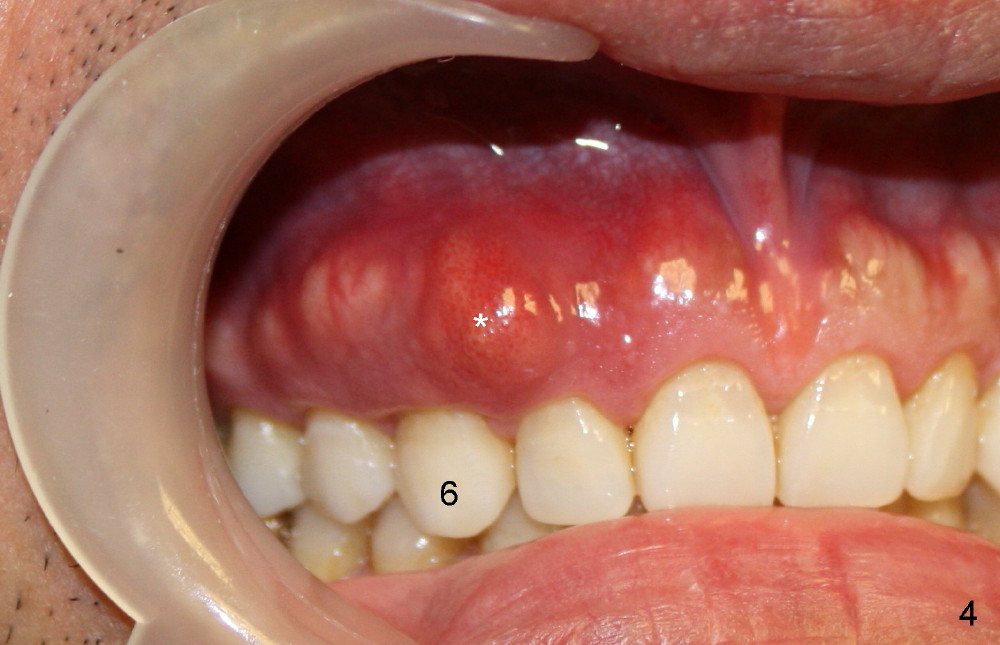
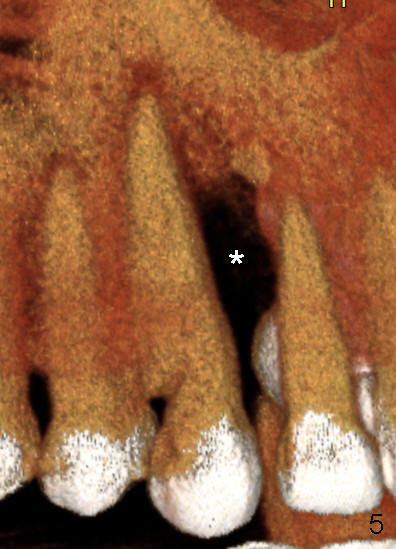
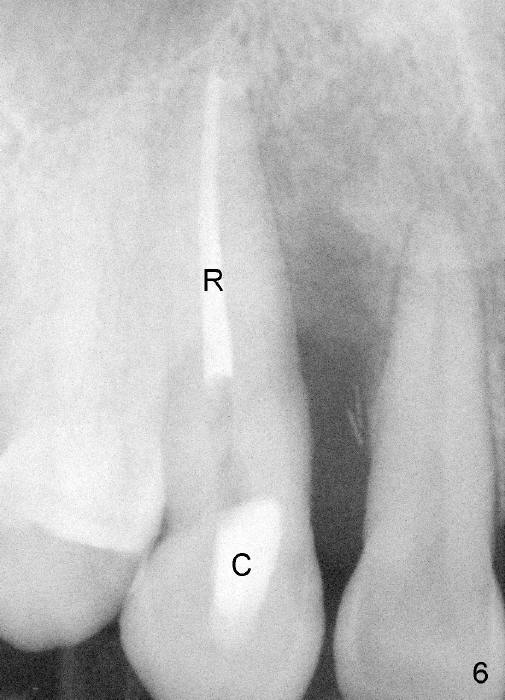
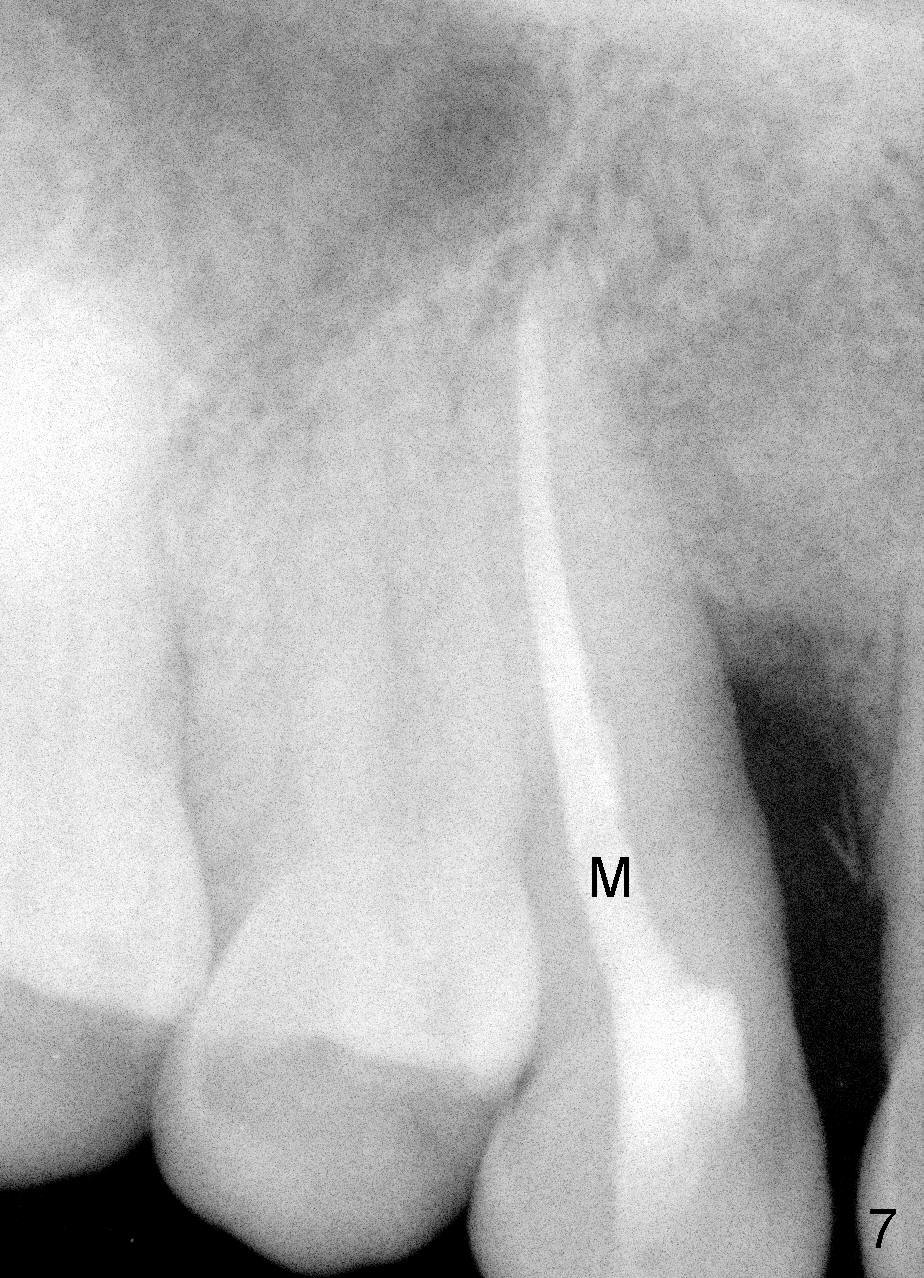
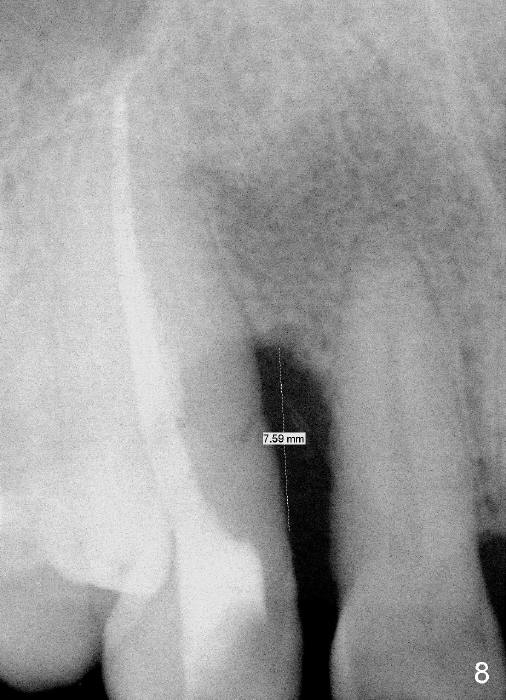
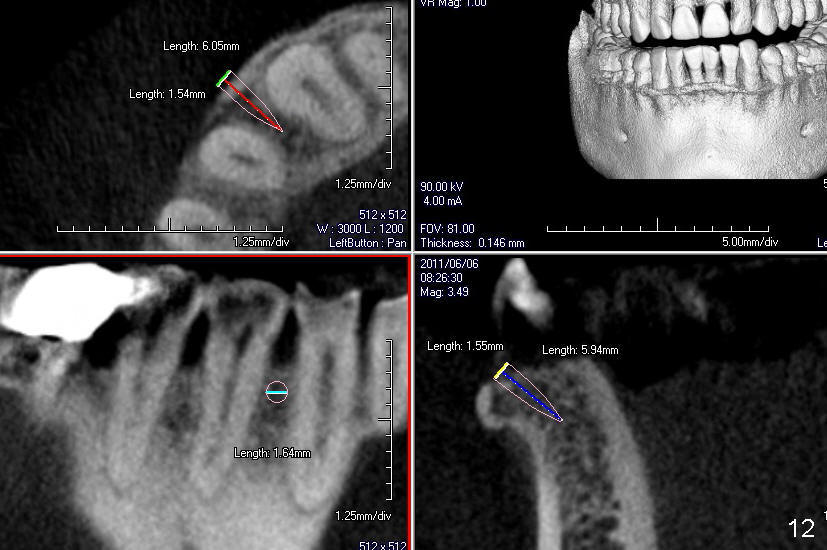
A male patient had trauma to the tooth #6 at the age of 13. The affected tooth has remained asymptomatic for more than 30 years (Fig.1). X-ray reveals an oblique root fracture (Fig.2 >) with radiolucency in the mesial alveolus (*, apparently normal trabecular pattern). Six years later (Feb. 2011), an acute infection develops (Fig.4 *). It requires incision & draining and antibiotic. At that time, the trabecular pattern disappears around the fracture line mesially (Fig.3 *). Four months later cone beam CT shows bone loss between #6 and 7 (Fig.5 *). Root canal therapy is done as a palliative measure (Fig.6 R; C: Cavit). Three months later, MTA (mineral trioxide aggregate) is placed in the coronal canal next to the fracture line (Fig.7 M). It is hoped that MTA can promote nearby bone and cementum to regenerate to seal the fracture line. Four months after MTA application, there is no sign of bone regeneration (Fig.8). Bone is lost for approximately 7 mm.
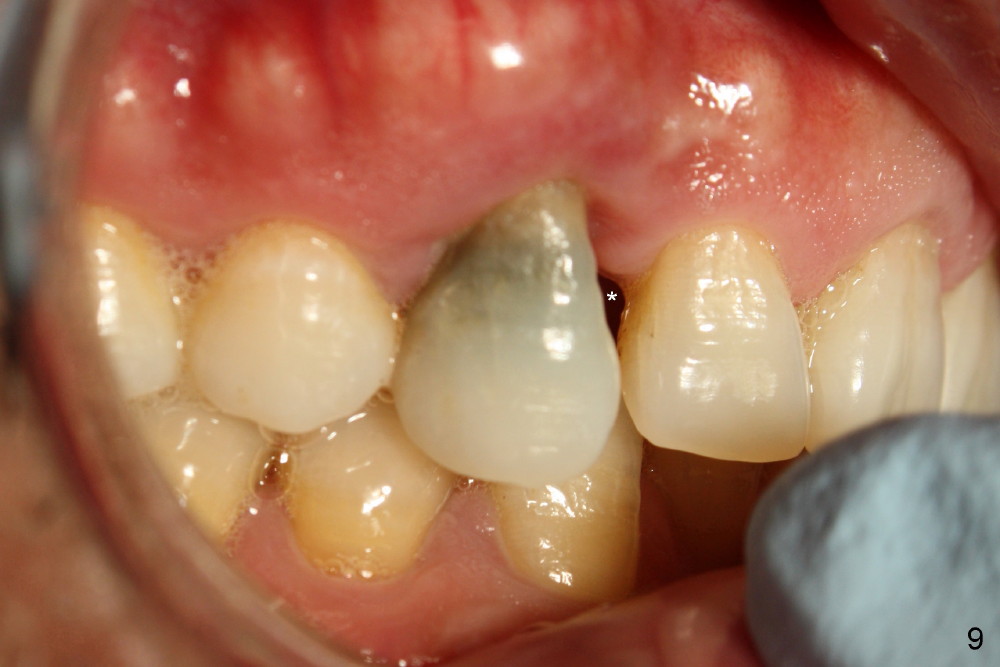
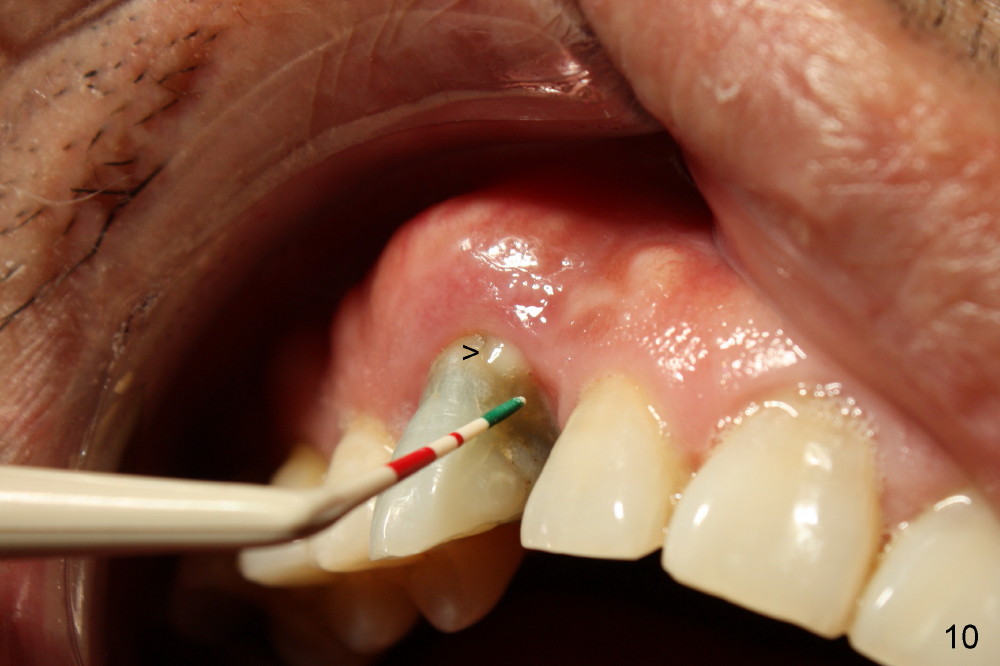
The tooth is discolored probably due to the side-effect of MTA(Fig.9; photo taken 9 months post-MTA). The mesial gingiva recedes (*). There is mild persistent pain with purulent discharge mesiobuccally (Fig.10 >). The corresponding pocket remains 7-8 mm deep in spite of root canal therapy and MTA.
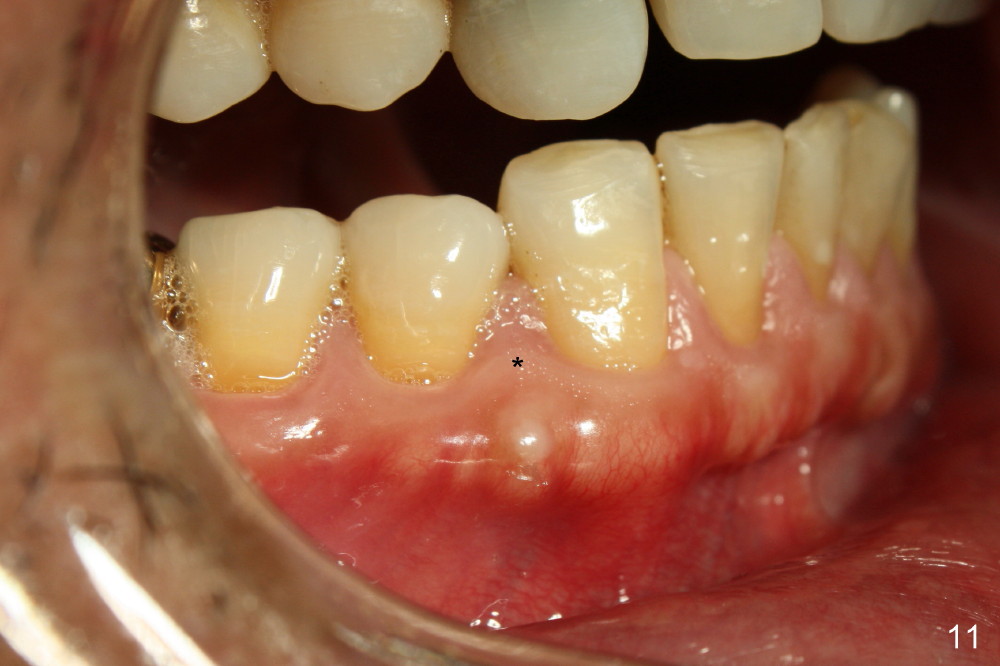
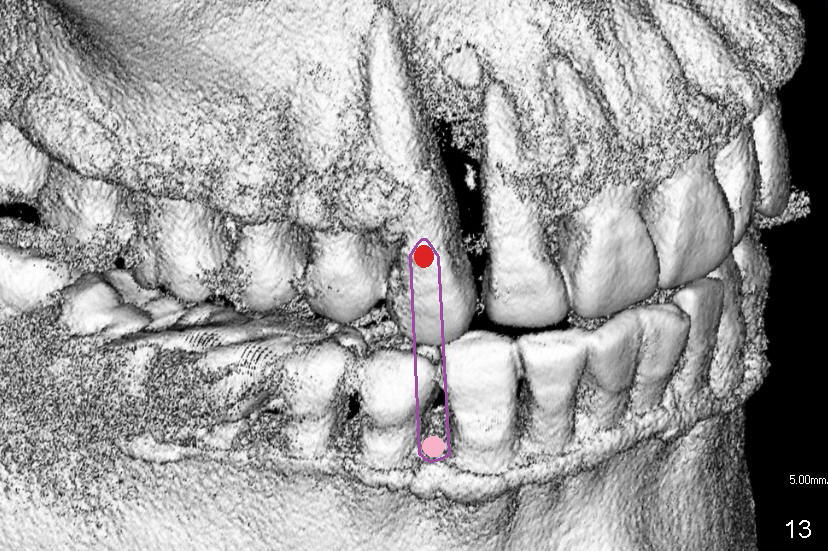
Treatment plan is to extrude #6 by placing a mini-implant between #27 and 28 (Fig.11-13) until the fracture line is exposed and the chronic infection is controlled. The most importantly, the extrusion is expected to bring down the mesial papilla and the alveolar bone. If the remaining root is not stable, the tooth is extracted and replaced by an implant.
What size of elastic is used? Brackets should be placed next to #6?
Progress of the case.
Xin Wei, DDS, PhD, MS 1st edition 09/23/2013, last revision 05/16/2014