
%2035%20ncm,%203.5%20m%20postop.jpg)

 |
 |
 |
 |
 |
 |
 |
 |
 |
%2035%20ncm,%203.5%20m%20postop.jpg) |
 |
 |
 |
Guide-Assisted One-Staged Ridge Split
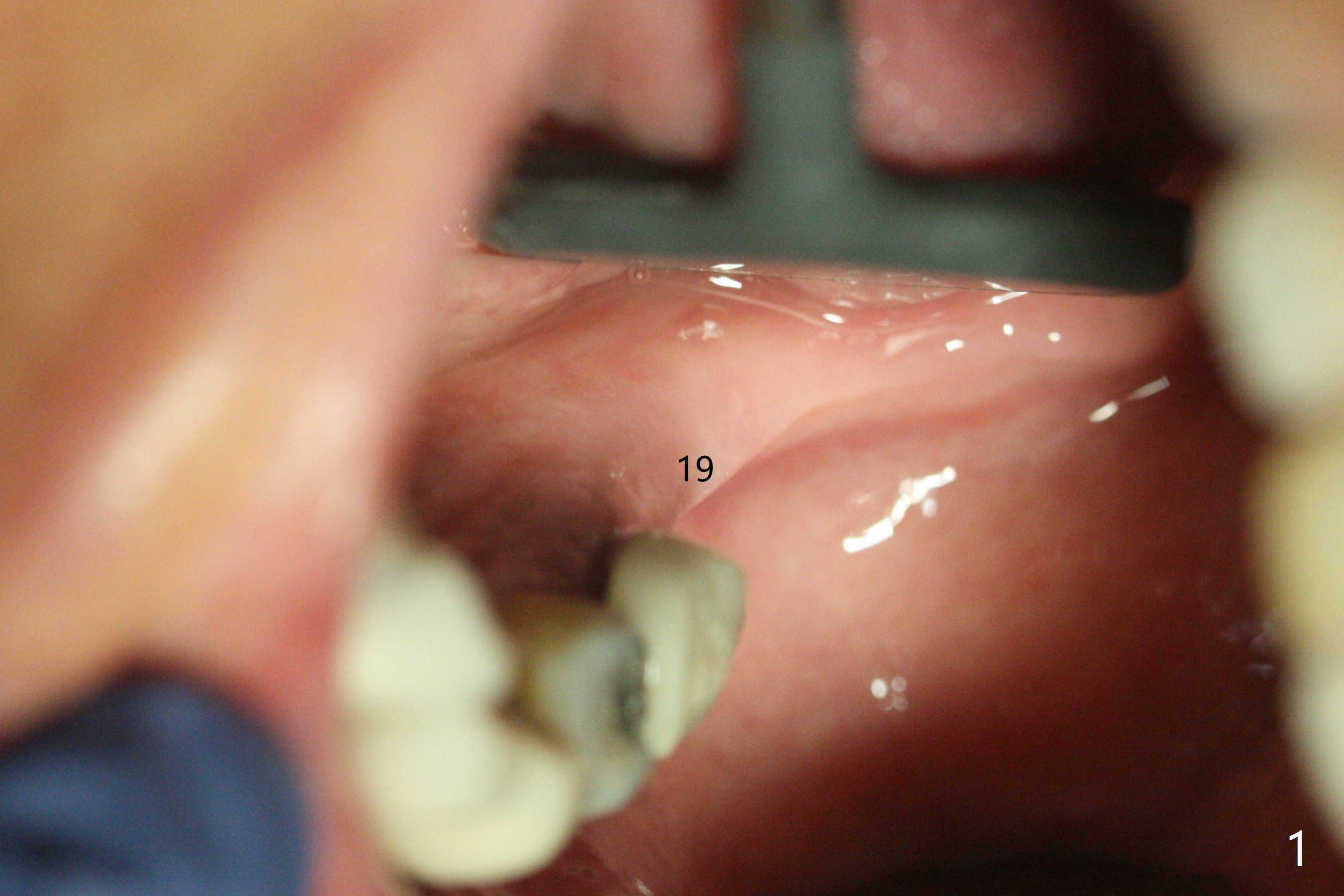
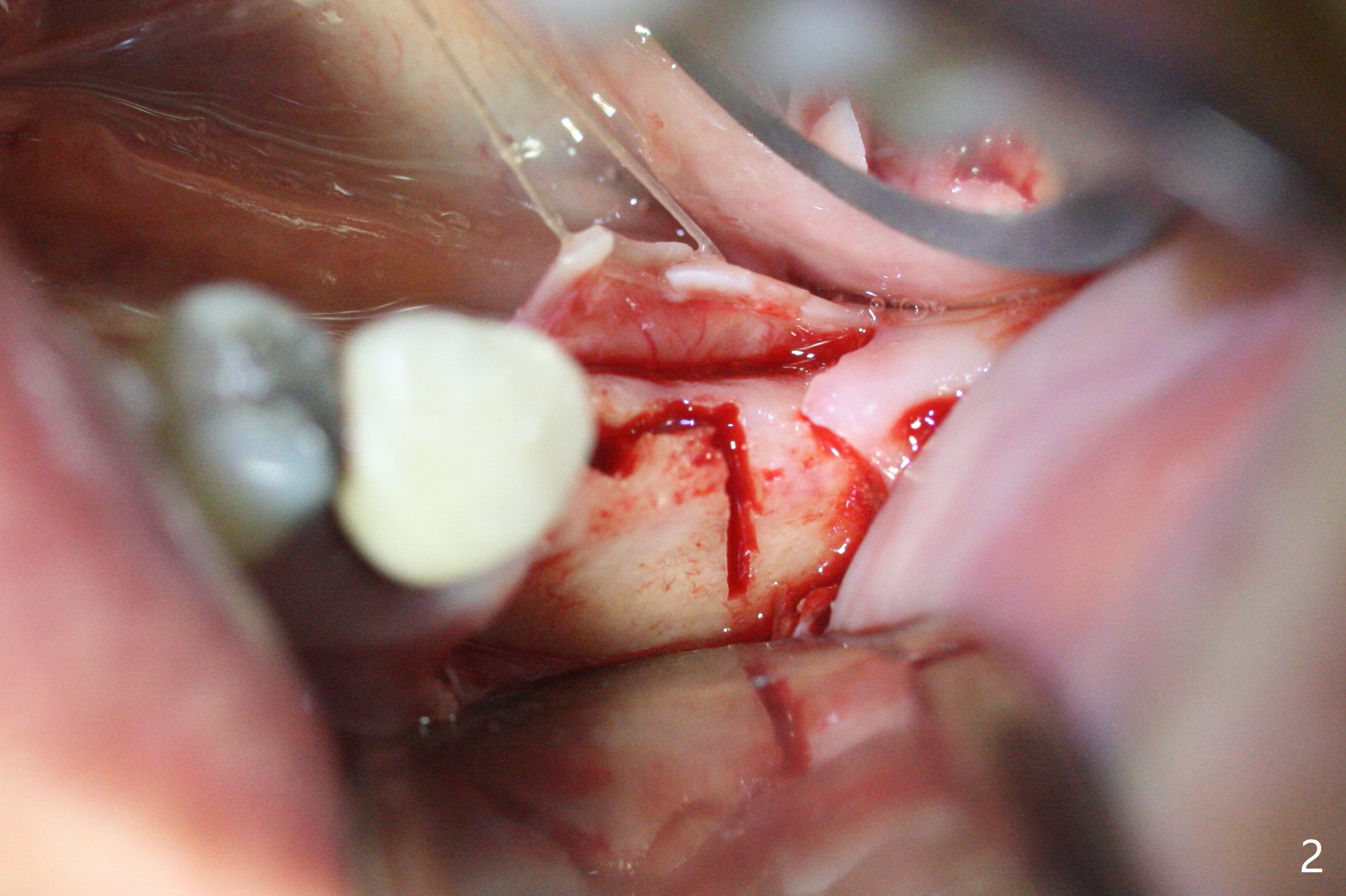
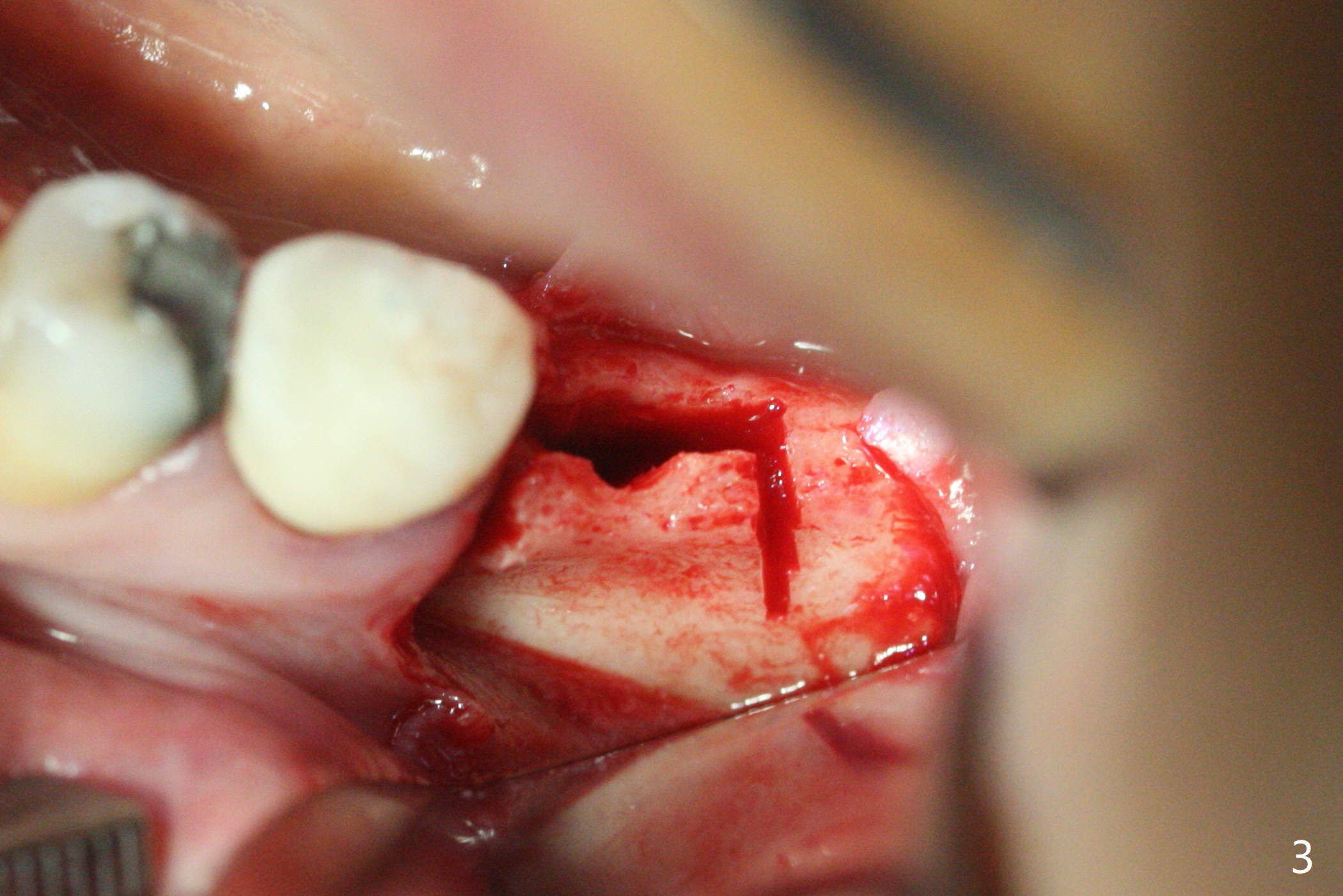
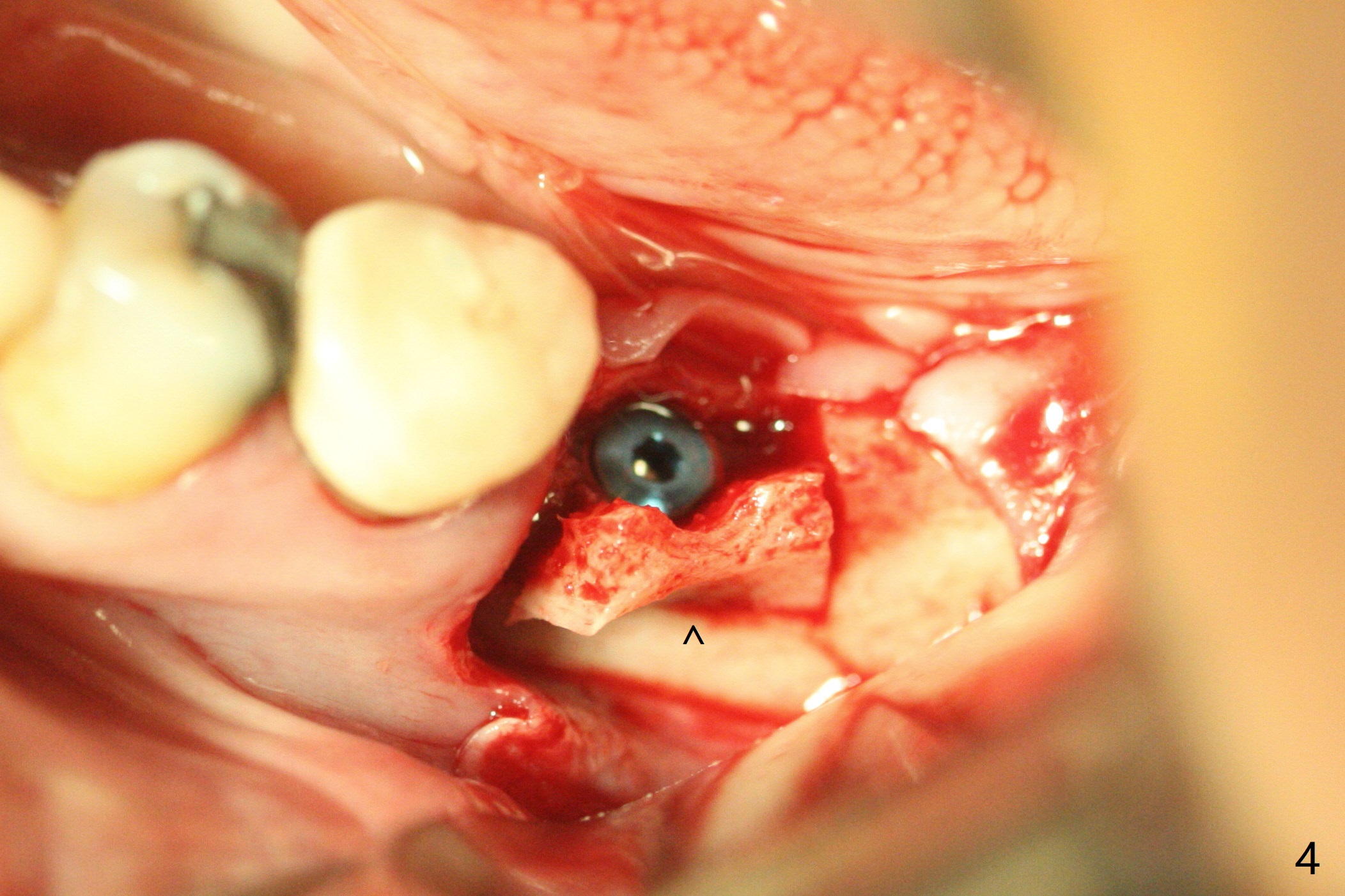
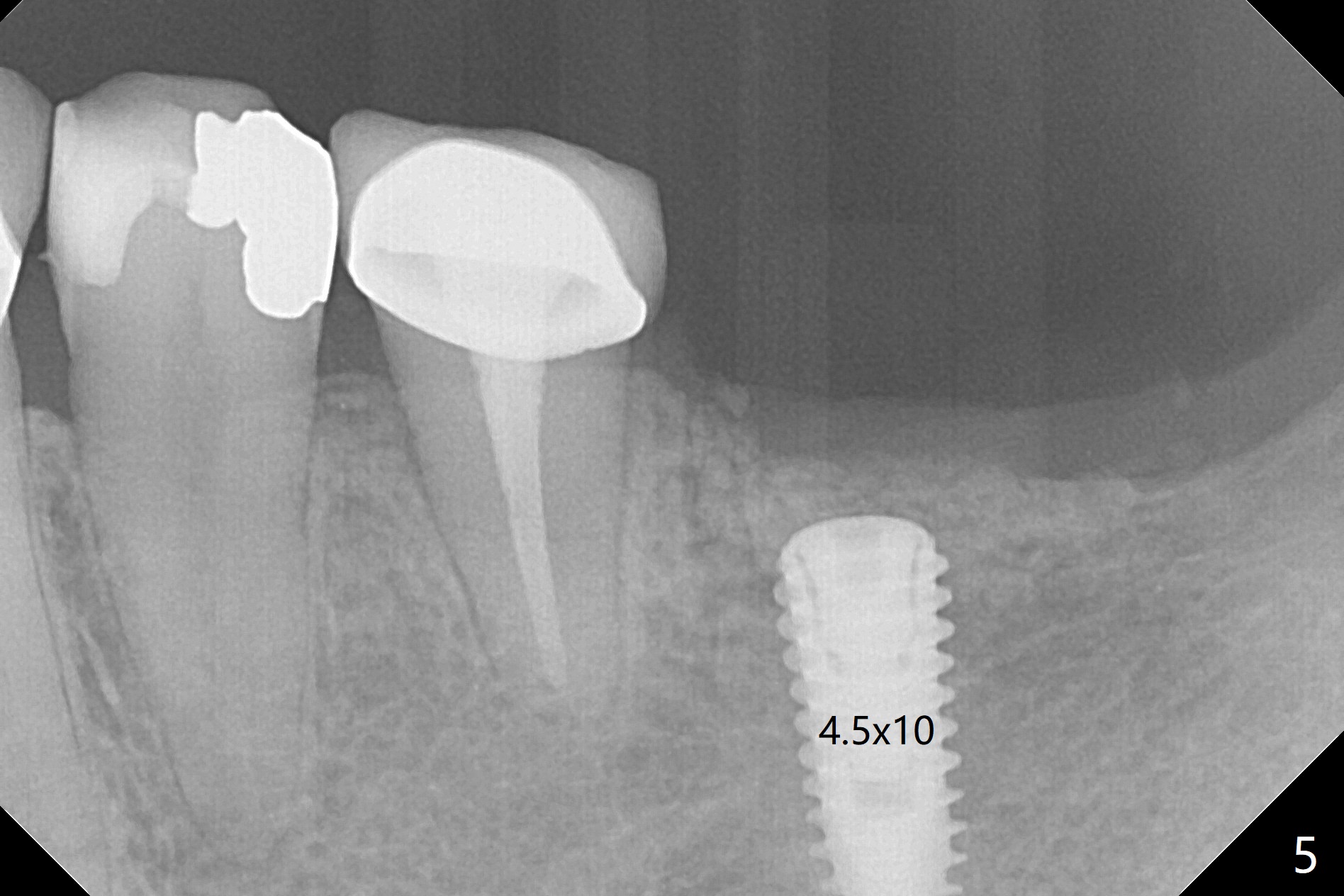
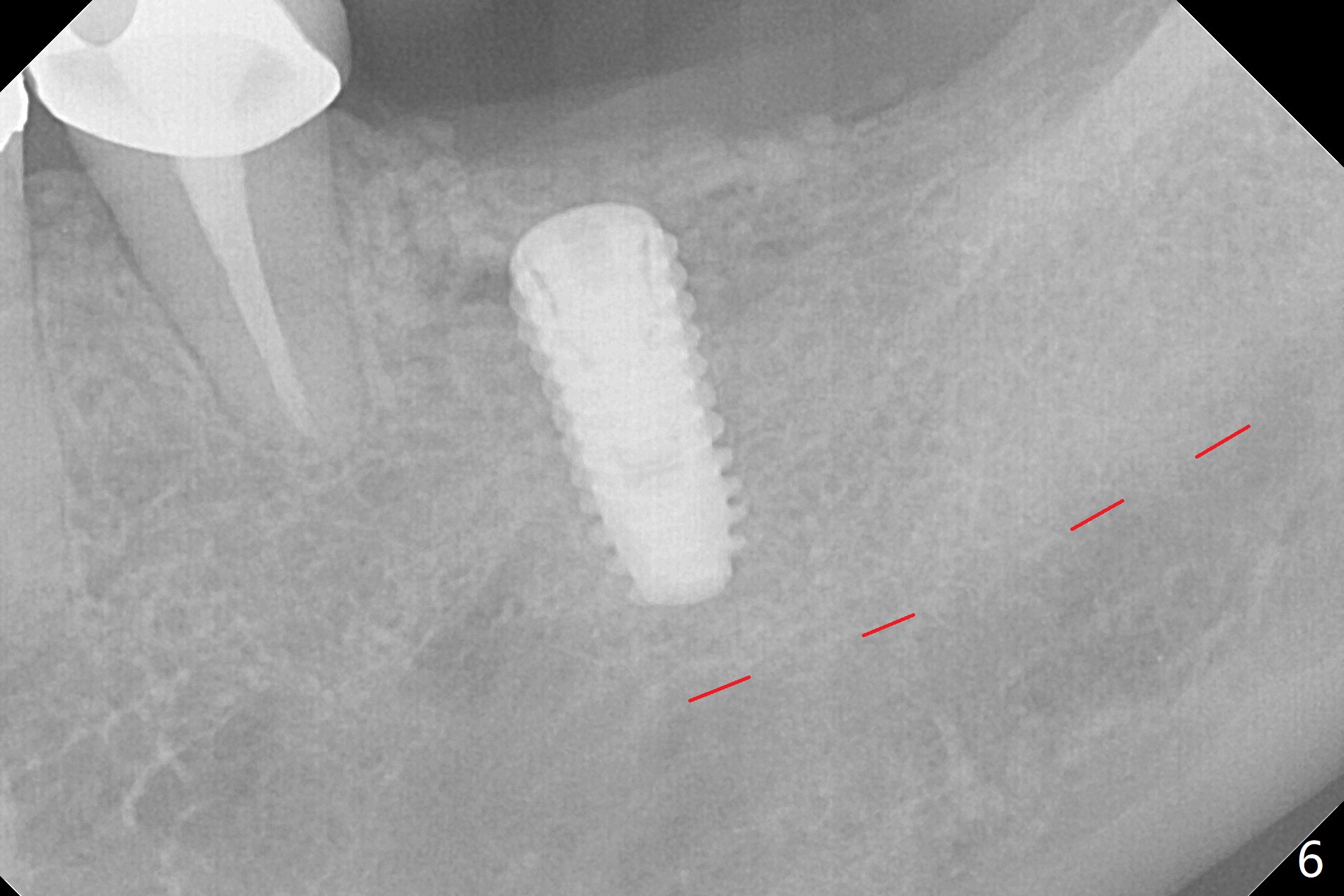
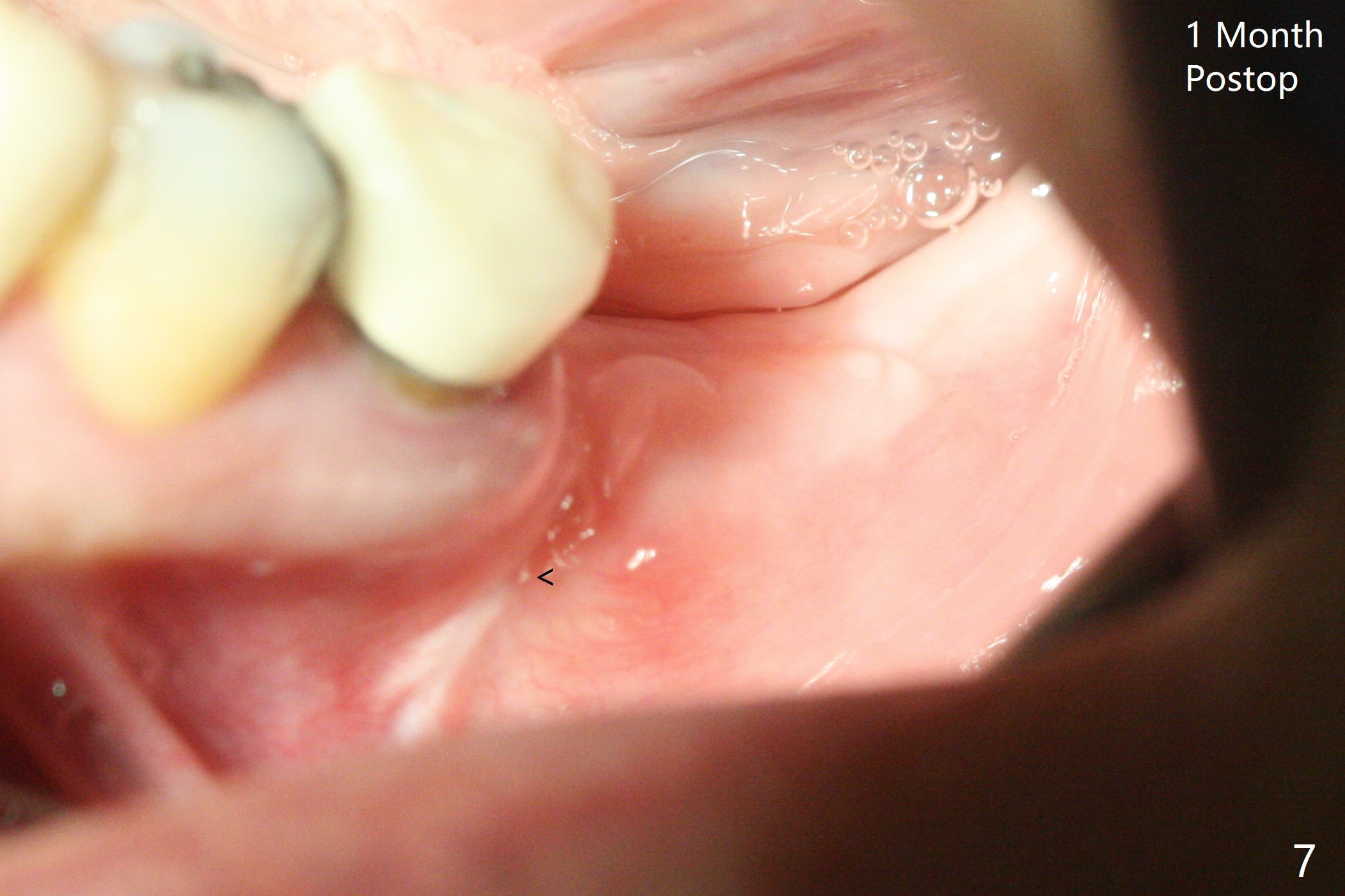
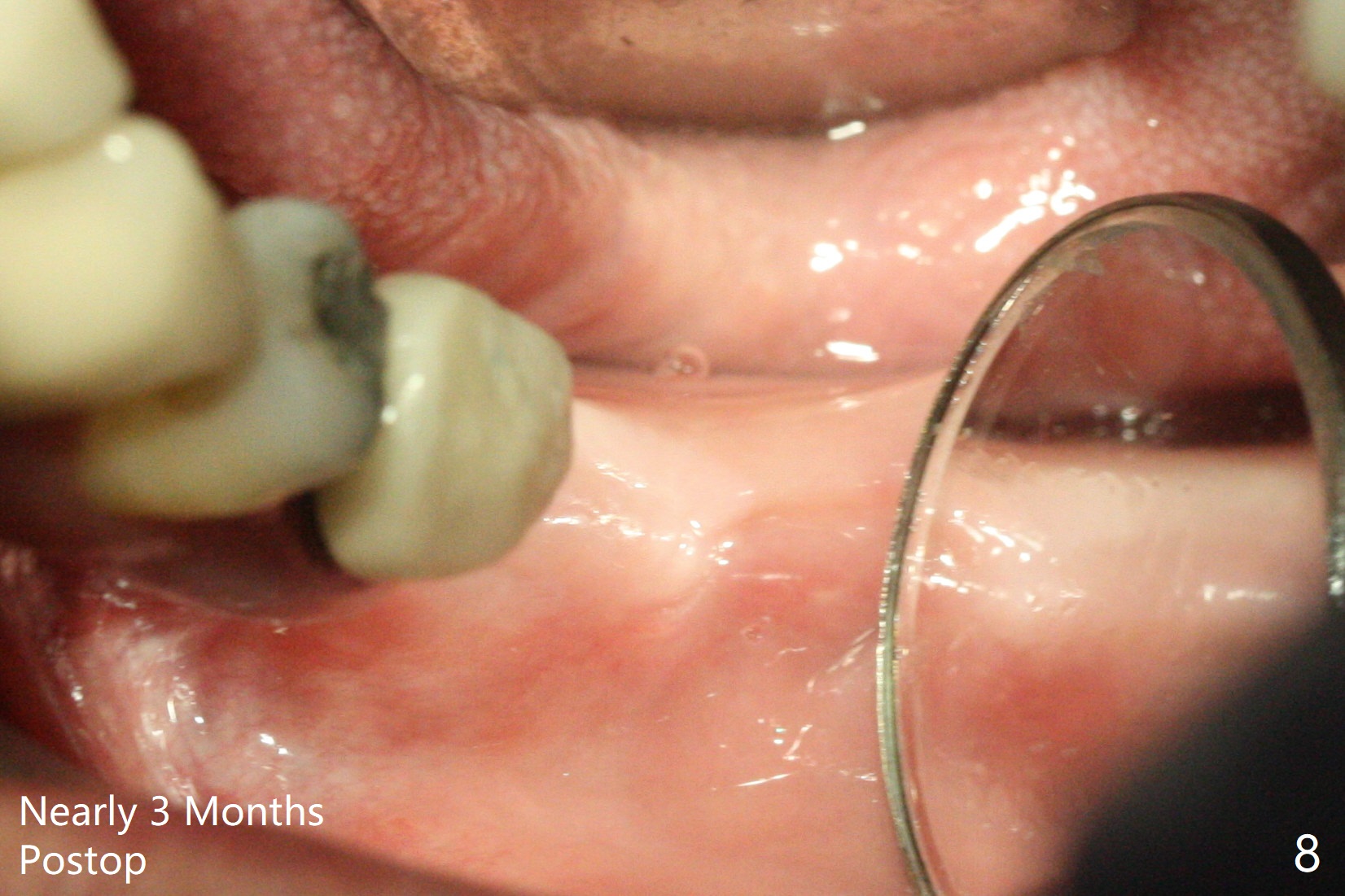
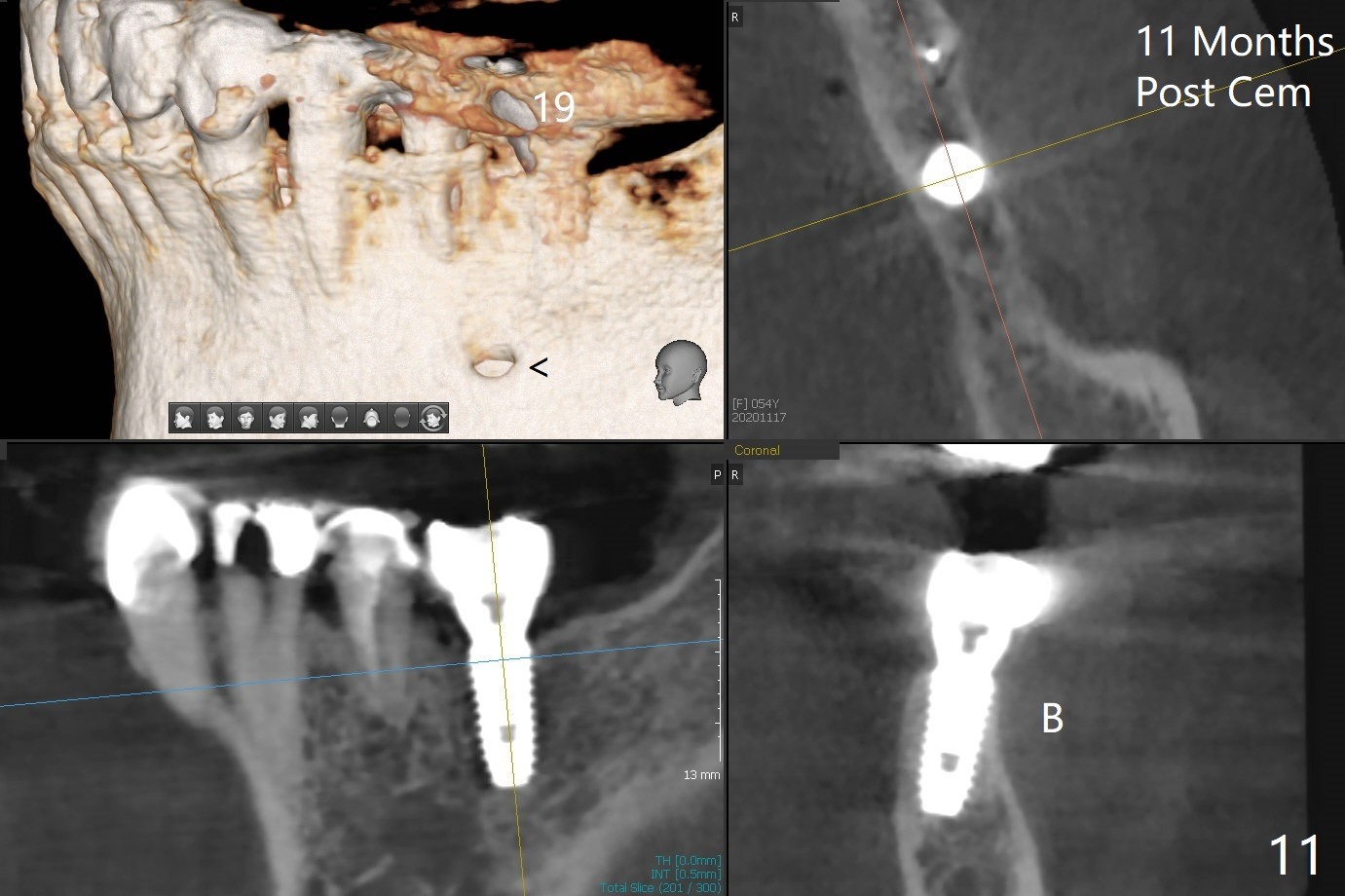
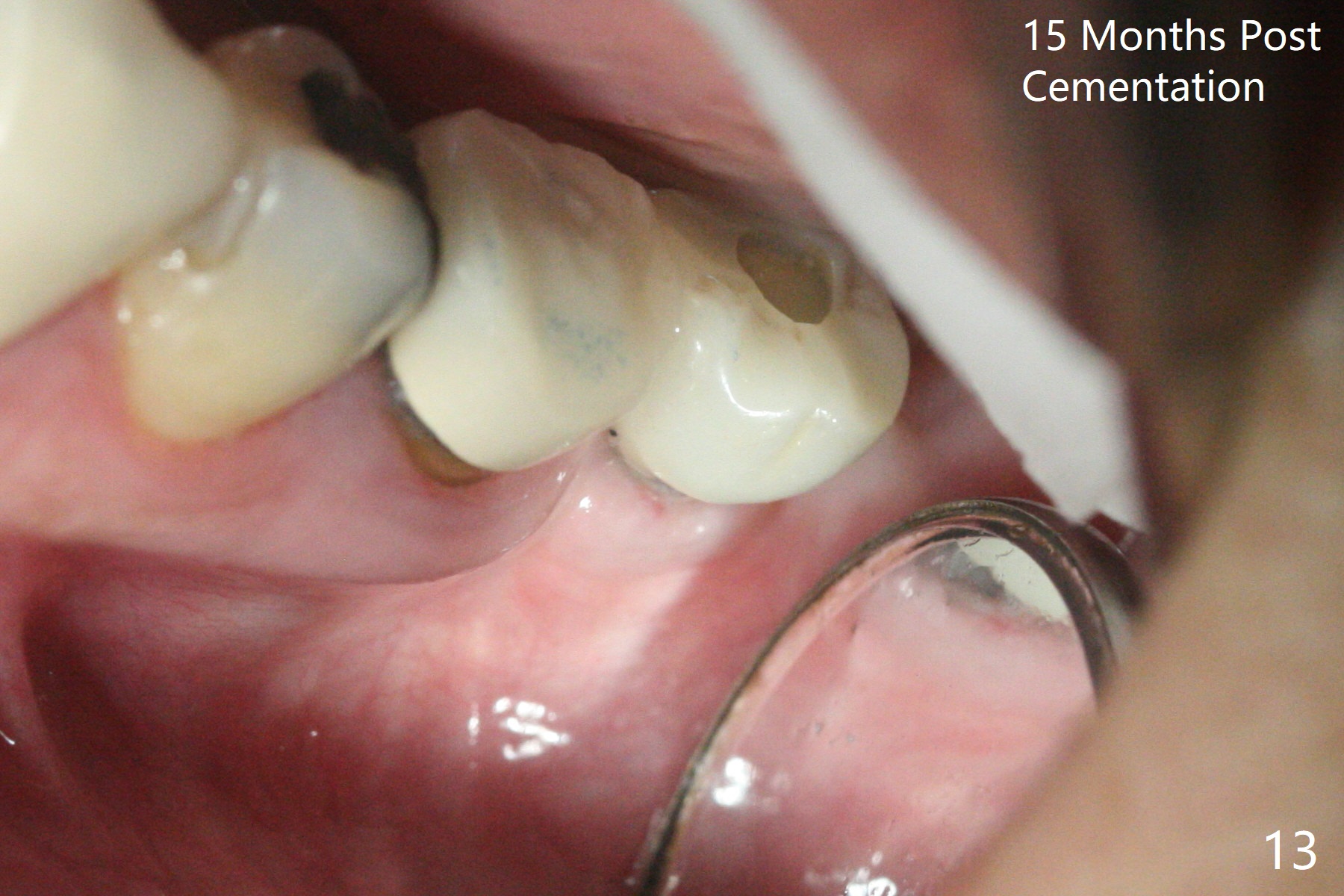
The ridge at #19 is narrow (Fig.1). After incision and initial osteotomy using 2.2 mm drill for 10 mm with guide, surgical handpiece and fissure bur are used for bony cuts (Fig.2). The ridge is split with bone scalpels and blades (Fig.3). The guide is reseated for final drilling until 3.5x10 mm. The buccal plate starts to fracture when a 4x10 mm IS dummy implant is being inserted; the fracture gets worse when a 4.5x10 mm final UF implant is placed (Fig.4 ^). Allograft is placed around the fracture before suturing (Fig.5,6). To prevent potential buccal plate necrosis, the procedure should be terminated when the ridge is initially split (Fig.3) and restart in 3 weeks. Periodontal dressing dislodges a few days postop with wound dehiscence in the buccal accessory incision area (Fig.4). Periodontal dressing is reapplied with one more week of oral antibiotic. Another complication is Mental Nerve paresthesia, associated with overzealous dissection before suture closure. The accessory incision dehiscence heals 1 month postop (Fig.7 <). The paresthesia seems to have been reduced. The ridge at #19 looks wider than that at #18 nearly 3 months postop (Fig.8). The split ridge appears to have healed (Fig.9). In uncover, the implant plateau is covered with bone; surgical handpiece is used to remove the overlying bone before removing the healing screw. Bone loss in the near future is expected to be minimal if more implants can be placed on the right side. The tooth #20 develops lingual abscess when the patient returns for abutment placement 3.5 months postop (Fig.10 *). Extraction and implant are apparently needed. The buccal plate is present, although thin 11 months post cementation (Fig.11,12). Although the buccal plate remains atrophic, the buccal soft tissue is healthy with sufficient keratinized gingiva 15 months post cementation (Fig.13).
Return to Lower Molar Immediate Implant, Trajectory II 3 11 12 Next 2-staged Ridge Split 劈开术
Xin Wei, DDS, PhD, MS 1st edition 08/24/2019, last revision 04/11/2021